In so many programs and dietary frameworks pushed on IBDers, the perspective revolves around which foods to exclude from one’s diet; however, in our approach to IBD, we focus on helping clients develop their own custom dietary framework with a focus on which foods to include. These are foods that promote healing, not just prevent damage, and the incredible superfoods that contain flavonoids are a spectacular example of this.
What are Flavonoids?
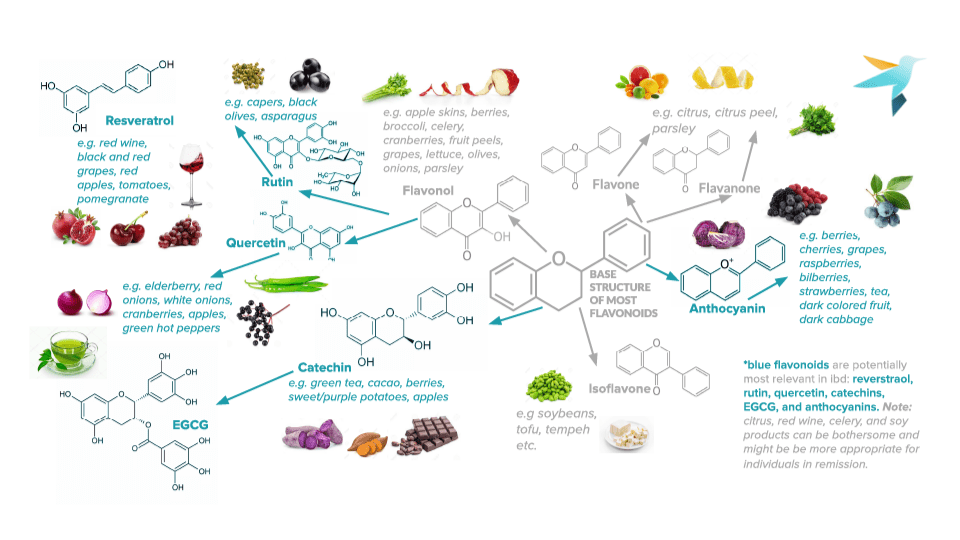
Polyphenols like flavonoids are known to have a variety of antioxidant and anti-inflammatory properties that may both decrease the risk of developing diseases like IBD and improve long-term disease outcomes.1,2 Part of an emerging area of nutrition research, flavonoids refer to a large class of bioactive compounds found in plants that may play a role in regulating the inflammation associated with IBDs like Crohn’s disease (CD), ulcerative colitis (UC), and microscopic colitis (MC).3 Flavonoids are easy to incorporate into the diet: they are present in most plant-based foods, with especially high proportions in colorful foods such as berries, tea, broccoli, and even dark chocolate! They are also the main bioactive component in some of the herbs we talk about here at IBDCoach including licorice, ginger, and ginseng.

In nature, flavonoids are responsible for the color and aroma of many plant-based foods, but they also serve an important role in plants’ self-defense against threats like microbes, UV radiation from the sun, and extreme climates like drought and frost. These compounds also impart protective properties to humans when ingested and consumed by our intestinal microbiota. These properties translate to immunomodulatory, anti-inflammatory, antioxidant, and prebiotic benefits that can further impact the gut microflora balance and intestinal barrier strength, all of which are important factors in IBD. Let’s take a closer look at a few of the well-studied types of flavonoids and what the research can mean for you and your gut health.
Flavonoids are Prebiotics for the Gut Microbiota
It is estimated that 90% of a person’s total dietary intake of polyphenols like flavonoids bypasses both digestion and absorption in the small intestine and are instead metabolized by the microbiota of the colon. Flavonoids feed our gut microflora and act as a prebiotic to support many beneficial gut microbes. This process sets off a chain reaction of secondary bioactive metabolites produced when the microbes consume the flavonoids. Those secondary metabolites support other helpful gut microbes, all of which can benefit dysbiosis-related diseases like IBD where the gut microbiome is known to be out of balance. In one animal study modeling colitis, the flavonoid compound resveratrol increased the beneficial bacteria Bifidobacterium and Lactobacillus while reducing Enterobacteriaceae (a family of bacteria commonly associated with intestinal upset).4 Catechins, a sub-category of flavonoids, stabilize the gastrointestinal tract environment by promoting the proliferation of beneficial intestinal bacteria, regulating the activity of intestinal flora, and potentially regulating tight junctions in the gut epithelium.5 Curcumin improved intestinal permeability and butyrate production by microbes in an animal study modeling IBD.4,6 As for human trials, curcumin has been able to prolong remission in UC patients with quiescent UC.5,6 Together, these studies promote the idea that flavonoids may be a powerful tool in the management of inflammatory bowel disease.
Read More About the Role of the Gut Microbiome in IBD
Evidence Linking Different Flavonoids and IBD
Both in vitro and animal studies help highlight some of the mechanisms by which flavonoids influence the activity of inflammatory mediators in IBD. Indonesian pomegranate peel, rich in anthocyanins and other polyphenols, both attenuated the expression of proinflammatory cytokines (such as TNF-ɑ and IL-IB) and enhanced the butyrate-producing bacteria Ruminococcaceae in an animal model of UC.7,8 Butyrate, a secondary metabolite, is a key fuel source for the colonocytes that make up the lining of the gut and therefore plays an essential role in maintaining the intestinal barrier in inflammatory bowel disease. In murine models, the natural flavone chrysin has demonstrated inhibitory effects on inflammatory mediators (to reduce inflammation) and ameliorative effects on the disrupted colonic architecture.9 Furthermore, flavonoids like quercetin, rutoside, morin, and hesperidin all alleviated diarrhea symptoms seen in experimental IBD by improving intestinal barrier function.10–13
While more research has been performed in animal models than in humans, a limited group of human studies shows promising results. One clinical trial using pomegranate (Punica granatum) peel extract demonstrated that consumption of these flavonoids reduced IBD symptoms of incontinence and need for antidiarrheals after four weeks when compared to a placebo group.14 Another trial treated thirteen UC patients with an anthocyanin-rich bilberry mixture, and after 6 weeks, subjects saw a significant reduction in mucosal inflammation and fecal calprotectin. While meaningful, those improvements were partially reversed by a follow-up report 4 weeks after the participants stopped the intervention. This outcome suggests that the therapeutic effects of flavonoid treatment for IBD may be transient and continuous consumption may be required.15 Still, these studies together provide a wealth of evidence that supports the potential benefits of consuming more polyphenols and flavonoids for inflammatory bowel disease.
Takeaways
Here at IBDCoach, we strive to uncover and present to you the latest research on IBD therapeutics so you can be informed and build a rounded protocol to achieve remission from IBD. Flavonoids can alter our immune responses, improve our intestinal barrier, and reshape our microbiota. These compounds are abundant in foods, from the purple-producing anthocyanins in blueberries, blackberries, and red cabbage, to the catechins found in green tea, cacao (dark chocolate), apples, legumes, and even some nuts like almonds and pistachios. These foods can be consumed in their whole form or in powders and extracts depending on what is the most feasible for you and your IBD. When combined with other interventions, a flavonoid-rich diet may help mitigate symptoms of IBD during a flare and even help prolong robust periods of remission. One thing is clear: flavonoids are a powerful and delicious prebiotic for inflammatory bowel disease.
Interested in learning what other factors support a robust Remission Master Plan to help you achieve remission from inflammatory bowel disease? Attend our FREE Microcourse: The Foundations of Remission today and learn about how to overcome your symptoms of IBD and build an individualized treatment protocol.
- Larrosa, M. et al. Effect of a low dose of dietary resveratrol on colon microbiota, inflammation and tissue damage in a DSS-induced colitis rat model. J. Agric. Food Chem. 57, 2211–2220 (2009).
- Fan, F.-Y., Sang, L.-X. & Jiang, M. Catechins and Their Therapeutic Benefits to Inflammatory Bowel Disease. Mol. J. Synth. Chem. Nat. Prod. Chem. 22, (2017).
- Curcumin Maintenance Therapy for Ulcerative Colitis: Randomized, Multicenter, Double-Blind, Placebo-Controlled Trial – Clinical Gastroenterology and Hepatology. https://www.cghjournal.org/article/S1542-3565(06)00800-7/fulltext.
- H, K. et al. Pomegranate polyphenolics reduce inflammation and ulceration in intestinal colitis-involvement of the miR-145/p70S6K1/HIF1α axis in vivo and in vitro. J. Nutr. Biochem. 43, 107–115 (2017).
- Kusmardi, K., Hermanto, D., Estuningytas, A., Tedjo, A. & Priosoeryanto, B. P. The Potency of Indonesia’s Pomegranate Peel Ethanol Extract (Punica Granatum Linn.) As Anti-inflammatory Agent in Mice Colon Induced by Dextran Sodium Sulfate: Focus on Cyclooxygenase-2 and Inos Expressions Asian J. Pharm. Clin. Res. 370–375 (2017) doi:10.22159/ajpcr.2017.v10i12.21390.
- Shin, E. K., Kwon, H.-S., Kim, Y. H., Shin, H.-K. & Kim, J.-K. Chrysin, a natural flavone, improves murine inflammatory bowel diseases. Biochem. Biophys. Res. Commun. 381, 502–507 (2009).
- Crespo, M. E., Gálvez, J., Cruz, T., Ocete, M. A. & Zarzuelo, A. Anti-inflammatory activity of diosmin and hesperidin in rat colitis induced by TNBS. Planta Med. 65, 651–653 (1999).
- Sánchez de Medina, F., Gálvez, J., Romero, J. A. & Zarzuelo, A. Effect of quercitrin on acute and chronic experimental colitis in the rat. J. Pharmacol. Exp. Ther. 278, 771–779 (1996).
- Gálvez, J. et al. Rutoside as mucosal protective in acetic acid-induced rat colitis. Planta Med. 63, 409–414 (1997).
- Ocete, M. A. et al. Effects of morin on an experimental model of acute colitis in rats. Pharmacology 57, 261–270 (1998).
- Kamali, M. et al. Efficacy of the Punica granatum peels aqueous extract for symptom management in ulcerative colitis patients. A randomized, placebo-controlled, clinical trial. Complement. Ther. Clin. Pract. 21, 141–146 (2015).
- Biedermann, L. et al. Bilberry ingestion improves disease activity in mild to moderate ulcerative colitis – an open pilot study. J. Crohns Colitis 7, 271–279 (2013).
- Ohno, M. et al. Nanoparticle curcumin ameliorates experimental colitis via modulation of gut microbiota and induction of regulatory T cells. PloS One 12, e0185999 (2017).